By ZMT Primary Healthcare Network |
zmtclinics.org
Think about the last time you were genuinely unwell.
Not just a brief headache — but something that worried you. Something you weren’t sure about. A symptom you couldn’t explain.
Who did you think of calling?
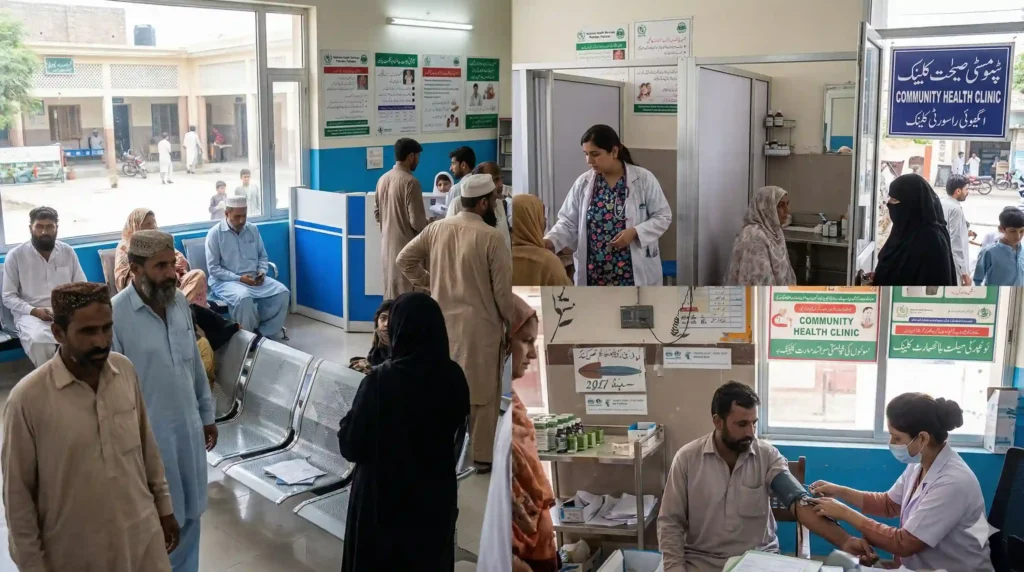
For people in affluent areas of Karachi, the answer is often a family doctor — someone who knows your history, understands your context, and gives you guidance you can trust. For millions in Karachi’s underserved communities, there is no such person. There is no one who knows their health history. No one who tracks their chronic conditions. No one who coordinates their care or advises them about when to worry and when to wait.
This is one of the most underappreciated dimensions of healthcare inequality in Pakistan: the absence of the family doctor.
At ZMT Clinics, we believe in the power of the family doctor model — and we’re building it, one clinic at a time, in the neighborhoods that need it most. This article explains what family doctors do, why they matter, and why they are the cornerstone of effective primary healthcare — particularly for communities served by Zakat and Sadaqah-funded organizations like ours.
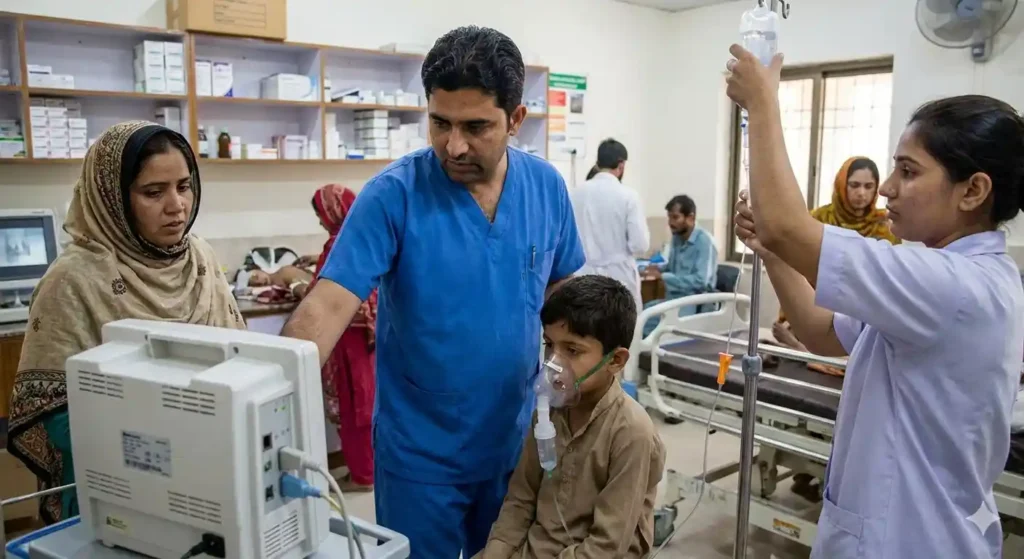
What Is a Family Doctor?
The term “family doctor” is used loosely in everyday conversation, but in healthcare terms it refers to a specific type of physician — one trained in family medicine or general practice — who provides:
- Continuous care: The same doctor over months and years, building a longitudinal relationship with the patient
- Comprehensive care: Managing the full range of health issues across age groups and organ systems, rather than focusing on one specialty
- Coordinated care: Serving as the central coordinator of a patient’s health journey — knowing when to refer, to whom, and ensuring follow-through
- Community-oriented care: Understanding the social, economic, and cultural context in which patients live
A good family doctor is, in essence, your personal health navigator — someone who knows not just your diagnoses, but your life circumstances, your family history, your anxieties, and your health goals.
This is fundamentally different from the fragmented, episodic care that most of Pakistan’s poor receive — where every visit to a different clinic means starting from scratch, and no one has the full picture.
Why Family Doctors Are the Backbone of Primary Healthcare
Every major healthcare system study reaches the same conclusion: countries with strong primary care and family medicine traditions have better health outcomes at lower cost.
The data is compelling:
- Countries with robust family medicine systems (UK, Netherlands, Australia, Canada) have significantly lower rates of preventable hospitalizations than countries where patients go directly to specialists.
- In the United States, where primary care is undervalued, studies show that increasing the ratio of primary care physicians to population by one per 10,000 people is associated with over 5% reductions in all-cause mortality.
- The World Health Organization consistently identifies strong primary care — centered on the family medicine model — as the foundation of Universal Health Coverage.
Why do family doctors produce these outcomes? Several reasons:
1. Continuity Catches What Single Visits Miss
A single clinic visit is a snapshot. Continuity of care is a film.
The pattern that reveals early diabetes — slightly elevated blood glucose readings over three consecutive visits — would be completely invisible if those three visits happened at three different facilities. The blood pressure that’s borderline one visit and elevated the next, prompting investigation — only visible to a doctor who sees the longitudinal record.
Family doctors, because they see the same patients over time, catch patterns. And patterns save lives.
2. Trusted Relationships Improve Patient Behavior
Research consistently shows that patients who have a trusted, continuous relationship with a primary care provider are:
- More likely to follow medical advice
- More likely to take prescribed medications consistently
- More likely to attend follow-up appointments
- More likely to seek care early rather than waiting until they’re in crisis
- Less likely to seek unnecessary emergency care
Trust is a clinical tool. A doctor you know and trust is worth more than the most sophisticated diagnostic technology used by a stranger.
3. Comprehensive Care Prevents Polypharmacy and Fragmentation
When patients see multiple specialists without a coordinating family doctor, they often end up on multiple medications — some of which interact. They receive duplicate tests. They receive conflicting advice. They fall through the gaps.
A family doctor is the hub that prevents this fragmentation — coordinating specialist inputs, managing medications holistically, and ensuring that the patient’s care makes sense as a whole.
4. Prevention Is a Core Commitment
Specialists, by their very nature, are focused on disease. Family doctors are focused on health — which means they invest in prevention, screening, and health promotion in a way that specialists simply do not.
For communities where the disease burden is primarily driven by preventable conditions — hypertension, diabetes, malnutrition, Hepatitis C — the preventive orientation of family medicine is extraordinarily valuable.
The Family Doctor Deficit in Karachi’s Underserved Communities
In Pakistan, family medicine is not adequately recognized or developed as a medical specialty. Most medical graduates aspire to specialist careers. Primary care is considered lower-status than hospital-based medicine.
The practical result: in Karachi’s affluent neighborhoods, every resident has access to multiple private GPs and family doctors within walking distance. In the slums of Orangi, Baldia, Korangi, and Lyari — which house millions of people — qualified family doctors are essentially absent.
This is not merely an inconvenience. It is a structural cause of preventable death.
As we’ve discussed in The Importance of Primary Healthcare for Karachi’s Underserved Communities, the communities that most need strong primary care are the communities least likely to have it. ZMT’s entire mission is to close this gap.
How ZMT Clinics Embody the Family Doctor Model
ZMT has built its clinical model around the principles of family medicine:
Qualified Physicians at Every Clinic
Every ZMT clinic is staffed by qualified medical officers (MBBS-trained doctors) who are supported by paramedical staff and nurses. While ZMT is growing toward having fully trained family medicine specialists at each clinic, the philosophy and approach of our clinical team is rooted in family medicine principles: comprehensive, patient-centered, continuous care.
Continuity Through the Patient Record
ZMT maintains patient records that allow the same patient to be recognized, tracked, and cared for consistently across visits. A patient who visits with hypertension is not starting from scratch at their next visit — their previous readings, medications, and history are available.
Comprehensive Scope
A ZMT clinic physician doesn’t just see one type of patient. In a single morning session, they might see a child with a respiratory infection, a pregnant woman for antenatal care, an elderly man for blood pressure management, and a young woman presenting with symptoms of depression.
This breadth is the defining feature of family medicine — and it’s how ZMT serves entire families, not just individual patients with specific conditions.
Integration with ZMT’s Specialty Programs
When a ZMT family physician identifies a patient who needs physiotherapy, mental health support, eye care, or Hepatitis C treatment, they have a direct pathway to refer within ZMT’s own specialty programs — all under the same roof or through the same network.
This integrated referral model means patients don’t fall through the gaps. The family doctor remains connected to the patient’s care even as specialists are involved.
To understand the full range of ZMT programs, read our Comprehensive Guide to ZMT Primary Healthcare Services.
What Does a ZMT Family Doctor Actually Do in a Day?
Let’s make this concrete. Here’s a picture of what a ZMT clinic physician manages across a typical day:
Morning Session:
- 7-year-old girl with recurrent ear infections → examined, antibiotic prescribed, mother counseled on hygiene practices
- 34-year-old woman, 20 weeks pregnant → antenatal visit, BP and hemoglobin checked, iron supplement continued, fetal growth assessed
- 58-year-old man with poorly controlled diabetes → glucose reading taken, medication adjusted, dietary counseling given, foot examined for neuropathy
- 2-year-old boy, brought in underweight → growth monitoring, malnutrition screening, referral to ZMT Malnutrition Program
- 45-year-old woman with chest tightness → ECG performed, hypertension identified, medication started, follow-up scheduled
Afternoon Session:
- New patient, 29-year-old woman presenting with fatigue and sadness → clinical assessment, depression suspected, referred to ZMT Mental Health Program with warm handover
- 65-year-old man with knee pain → clinical examination, physiotherapy referral arranged
- 12-year-old with school-related visual difficulty → vision screening, glasses prescription, referral to ZMT Eye Program
- Hepatitis C follow-up patient, week 8 of treatment → progress reviewed, adherence confirmed, next supply of antivirals dispensed
- 40-year-old construction worker with back pain — first presentation → clinical assessment, Red Flags ruled out, physiotherapy referral, work modification advice
This is family medicine in practice — comprehensive, continuous, community-embedded, and managing the full spectrum of human health needs.
The Relationship Between Family Doctors and Community Trust
In Pakistan’s underserved communities, there is a profound trust deficit around formal healthcare. Many residents have had experiences of dismissal, long waits, poor communication, or feeling that their concerns were not taken seriously.
Building trust is not a soft objective at ZMT — it is a clinical strategy.
When a patient trusts their doctor, they: – Come back for follow-up – Take their medicines correctly – Bring their children for immunization – Share symptoms they would otherwise hide – Follow preventive care advice
ZMT’s continued medical education program — which regularly trains and updates our clinical staff — includes not just clinical skills but communication skills, patient-centered care approaches, and cultural competency.
The goal is not just to diagnose and treat, but to be the trusted healthcare relationship that Karachi’s most vulnerable families have never had before.
Family Doctors as the Bridge to Specialist Care
An important and often invisible role of the family doctor is gatekeeping — deciding when specialist input is needed and facilitating access to it.
In communities without family doctors, this function fails. People either: – Never access specialist care when they need it (because they don’t know they need it), or – Access specialist care inappropriately and expensively for conditions that a GP could have managed
ZMT’s physicians serve this bridge function daily — identifying which patients need referral to ophthalmology, cardiology, obstetric specialist care, or any other specialty, and facilitating those referrals within ZMT’s network or to public hospital facilities.
As we explained in What Is Primary Healthcare and How Does It Differ From Tertiary Care?, the family doctor is the essential link between primary care and the higher levels of the healthcare system. Without this link, the system doesn’t function as a system at all.
Supporting Family Doctors Through Zakat and Charity
Running a clinic that embodies the family medicine model requires sustained investment:
- Qualified physicians who are paid fairly and supported professionally
- Medical records systems that enable continuity
- Comprehensive supplies: medicines, diagnostic equipment, consumables
- Ongoing training to keep clinical skills current
- A physical space that is dignified and welcoming
None of this is free. ZMT’s clinics run on the generosity of donors — individuals who give Zakat, Sadaqah, and voluntary charity.
When you direct your Zakat to ZMT, you are funding not just a single consultation, but the infrastructure of continuous care — the family doctor model that Karachi’s most vulnerable communities have been denied for generations.
In Islamic tradition, caring for the health of the vulnerable is among the highest acts of charity. The Prophet Muhammad (PBUH) said: “The best of people are those most beneficial to people.” Funding family medicine for those who have no alternative is precisely this kind of benefit — sustained, systemic, and deeply impactful.
ZMT is a recognized Zakat-eligible organization. Your giving is Islamically compliant and directly benefits eligible patients.
Final Thoughts
The family doctor is not a luxury of the affluent. In every well-functioning healthcare system in the world, the family doctor is the foundation — the continuous, trusted, comprehensive care provider who knows patients as whole people and manages their health across the arc of their lives.
Karachi’s underserved communities have been denied this foundation for too long. ZMT is building it — clinic by clinic, patient by patient, relationship by relationship.
If you live in Karachi and lack access to affordable primary care, ZMT’s clinics are open to you. No appointment needed. Walk in.
If you want to support the work of building family medicine for those who need it most, donate your Zakat or Sadaqah at zmtclinics.org.
And to learn more about all the services your donation supports — read our Top Primary Healthcare Services Offered at ZMT Clinics.
ZMT Primary Healthcare Network — Quality primary healthcare for every woman and child in Pakistan. Donate your Zakat and Sadaqah at zmtclinics.org

